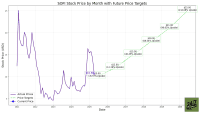
Goldman Sachs (NYSE:GS | GS Price Prediction) added UnitedHealth Group (NYSE:UNH) stock to its U.S. Conviction List, reiterating a Buy rating with a $435 price target. The firm argues UnitedHealth is nearing the bottom of its underwriting cycle in Medicare Advantage (MA), which represents 40% of its business.
The Conviction List is reserved for Goldman’s highest-conviction Buy ideas. UnitedHealth stock’s addition follows a powerful rebound: shares climbed 37% in April alone, the standout move across the managed care group.
For prudent investors, the call validates a thesis building since Q1 2026 earnings: the worst of the medical cost ratio (MLR) shock from 2025 may be behind us. The Q1 print showed MCR back to 83.9%, a meaningful improvement from the 2025 peak.
| Ticker | Company | Firm | Action | Old Rating | New Rating | Old Target | New Target |
|---|---|---|---|---|---|---|---|
| UNH | UnitedHealth Group | Goldman Sachs | Conviction List Add | Buy | Buy | $435 | $435 |
The Analyst’s Case
Goldman’s thesis hinges on the Medicare Advantage underwriting cycle bottoming. With MA representing 40% of UnitedHealth’s business, any inflection in pricing discipline and cost trends flows disproportionately to earnings.
Q1 2026 supports that view. UnitedHealth’s medical care ratio improved 90 basis points year over year (YoY) to 84%, and adjusted EPS came in at $7.23 versus the $6.61 consensus. UnitedHealth CFO Wayne DeVeydt attributed the improvement to “pricing discipline, strong medical cost management, and favorable reserve development.”
Bank of America (NYSE:BAC) also carries a Buy rating on UNH stock with a $435 target after its earlier price target raise tied to Medicare Advantage rate finalization, adding a second institutional voice to the bull case. Two top-tier firms now share the same target, reinforcing the institutional bid.
Company Snapshot
UnitedHealth operates through UnitedHealthcare and Optum, serving approximately 49.1 million medical members with Optum Rx processing roughly 383 million adjusted scripts per quarter. Q1 2026 revenue reached $111.72 billion, up 2% YoY.
Management raised UnitedHealth’s full-year 2026 guidance to greater than $18.25 in adjusted EPS, committed to at least $2 billion in share repurchases by the end of Q2 2026, and disclosed plans to invest nearly $1.5 billion in AI-related initiatives in 2026. The capital return commitment underscores management’s confidence in the recovery trajectory.
Why the Move Matters Now
UnitedHealth trades at a forward P/E ratio of 20x, with consensus analyst target at $387.27. Goldman’s $435 target sits above the consensus, signaling room for upward revisions if MA margins normalize.
The bear case remains real. Medicare Advantage membership declined 965,000 in Q1 2026, Medicaid membership contracted 220,000, and DOJ legal actions concerning Medicare participation remain unresolved. After a 37% April rally, the easy money has likely been made in UnitedHealth stock.
Yet, UNH stock is up 12% year to date (YTD) and remains 7.4% below its level a year ago, suggesting further upside if cost trends hold. That gap to prior highs frames the runway Goldman is targeting.
What It Means for Your Portfolio
Goldman’s Conviction List addition is a meaningful institutional signal, particularly paired with Bank of America’s matching $435 target and UnitedHealth’s 2.38% dividend yield backed by five consecutive years of double-digit dividend raises. The combination of analyst conviction and a growing dividend strengthens the total-return profile.
Prudent UNH stock investors shouldn’t chase the rally. Moderate position sizing makes sense given regulatory overhang, potential MA rate cuts in future cycles, and MLR pressure if utilization reaccelerates. UnitedHealth CEO Stephen Hemsley’s framing remains cautious, noting the company is still “continuing to help simplify and modernize health care” rather than declaring victory.
Watch for whether UnitedHealth’s Q2 2026 medical cost ratio holds near current levels, whether the Alegeus Technologies acquisition closes on schedule, and whether DOJ developments stabilize. Those data points could determine whether the managed care comeback is durable or a sharp mean-reversion bounce.